Background/Pathophysiology
Hypothyroidism, or an underactive thyroid, occurs when the thyroid gland does not produce enough thyroid hormone. The most common cause of hypothyroidism in Australia is Hashimoto’s disease, or thyroiditis. This is an autoimmune disease that occurs when the body’s immune cells attack the thyroid gland. If affects approximately 4-5% of the Australian population, predominantly women (who are 2-3x more likely to have it) and the elderly.
Other common causes of hypothyroidism include:
- Surgery that removes some or all the thyroid gland
- Radiation therapy
- Treatment for an overactive thyroid (hyperthyroidism)
- Some medicines, including lithium
It can also be caused by too little iodine in the diet, congenital disease, a problem with the pituitary gland, or by pregnancy.
Risk Factors
Although anyone can develop hypothyroidism, however, you’re at an increased risk if you:
- Are a woman
- Are older than 60
- Have a family history of thyroid disease
- Have an autoimmune disease, such as type 1 diabetes or celiac disease
- Have been treated with radioactive iodine or anti-thyroid medications
- Received radiation to your neck or upper chest
- Have had thyroid surgery (partial thyroidectomy)
- Have been pregnant or delivered a baby within the past six months
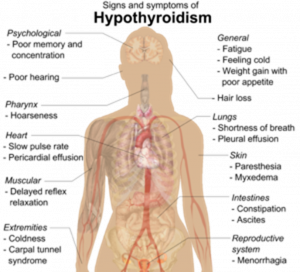
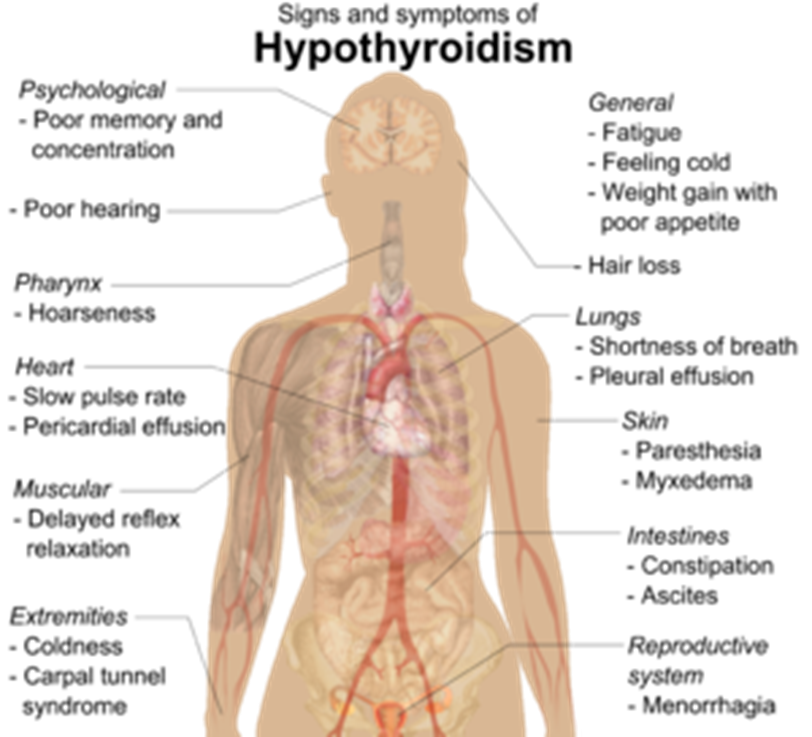
Presentation or symptoms
As the thyroid gland is involved in so many bodily processes that there is a lot of signs and symptoms that can occur when it is not functioning well. In saying that, hypothyroidism can also be present without experiencing any symptoms.
- Fatigue
- Poor tolerance to the cold
- Unexplained weight gain
- Puffy and pale face
- Brittle hair and nails, thinning hair, hair loss (of the outer third of the eyebrow in particular)
- Dry, cool skin
- Muscle pain
- Constipation
- Headaches
- Poor attention span or memory
- Slow heart rate
- Heavier than normal periods
- Depression
- Enlarged thyroid gland
Diagnosis
A doctor may check for nodules on the thyroid gland or a slow heart rate. Hypothyroidism is diagnosed through blood tests of the hormones T3, T4, and TSH.
- T3 (triiodothyronine) and T4 (thyroxine): while both molecules can trigger biological effects, T3 is considered the active thyroid hormone that binds to thyroid hormone receptors (TR), while T4 is a prohormone that must be converted to T3 in order to initiate signalling and gain biological activity
- TSH or thyroid stimulating hormone: is produced in the pituitary gland and stimulates the thyroid gland to produce more hormones
Common co-morbidities or Associated conditions
- Diabetes, Type 1 and 2
- Thyroid cancer
- Larynx cancer
- Hyperthyroidism
- Goitres
- Heart disease or heart failure
- Mental health disease
- Peripheral neuropathy
- Myxedema- result of long term, untreated hypothyroidism
- Birth defects
- Infertility
So where does exercise fit in all of this?
Well, while it is unknown if exercise impacts thyroid function directly, it has many impacts on the side effects and managing any changes in symptoms such as fatigue, muscle aches, and your mental health. Exercise recommendations for general health apply, 150 minutes of moderate intensity activity or 75 minutes of vigorous exercise per week with at least 2 days of resistance training. In saying this, recovery and an appropriately prescribed program are paramount in navigating symptoms such as fatigue and increased muscle and joint pain.
For those of you who have been already diagnosed, let your Accredited Exercise Physiologist know so an appropriate and effective program can be created with your goals in mind. I also urge you not to brush off changes in symptoms and consult your GP about further testing if you notice any changes.